In the last blog we touched upon a pathological dental process known as resorption. As discussed, resorption is a process in which tooth structure is ‘eaten away’ due to the body’s response when the tooth is subjected to trauma, an infection or other stimuli. We discussed two types of resorption, internal and external root resorption.
In this blog, we will continue our discussion of tooth/root resorption, so it may be best to reread the latter one to refresh your knowledge…here we go.
External root resorption
External resorption is more common than internal resorption. Root resorption most often starts from the outside of the tooth and works itself inwards.
Factors which cause external root resorption:
1) Orthodontics: Occurs when orthodontic forces applied to the teeth are excessive or when teeth are moved too quickly during the orthodontic process. We will discuss this concept in the next blog.
2) Injury or trauma: Trauma to the tooth can damage periodontal fibers (PDL fibers). These are sensory fibers which attach the root of the tooth to the bone. If these sensory fibers (also known as periradicular tissues) become disturbed by some sort of trauma to the tooth, then an inflammatory process can be initiated. This may lead to the start of external resorption. We will discuss PDL fibers in a future blog.
3) Infection.
4) Unknown etiology: Often occurs in the absence of a known cause.
Common location of external resorption – Most common in:
1) Upper front teeth: canines and incisors.
2) Lower first molars.
External resorption progressively gets worse over time. It initially shows up as a distinct dark spot on a routine x ray, but the resorption progresses very quickly. For this reason, it is important to treat it as soon as it is detected. Otherwise, the destruction/resorption may occur so rapidly that it may not be possible to save the tooth…saving the tooth will depend on the degree of destruction.
Treatment
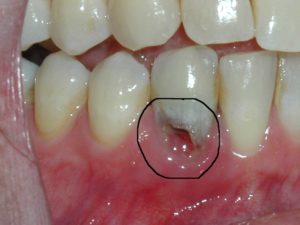
Treatment will depend on where the lesion (initial resorption) occurs. If the lesion is external and occurs just below the gums (see the above image), it is often possible to treat. One would need to ‘open’ up the area surgically, remove the damaged tissues/cells and repair the root with a white filling. If the resorption reaches the nerve of the tooth, a root canal procedure is usually required. If the resorption is too advanced, it is best to extract the tooth and place a dental implant. For more information on dental implants, please see the blog, “Dental Implants…A Great Solution for a Missing Tooth,” posted on October 9th, 2011.
Internal Tooth Resorption
The most common cause of internal root resorption is an infection within the pulp/nerve of the tooth. This causes stress on the dentin that make up the walls of the pulp chamber.
The infection results in the stimulation of an inflammatory process within the pulpal tissues which causes the internal resorption.
As mentioned previously, with both internal and external root resorption, the initial resorption can only be seen at its earliest stages on an x ray. As time goes by and the degree of resorption increases, the tooth may become symptomatic…this may present in the form of a periradicular abscess (an abscess around the root of the tooth) and increased tooth mobility.
Again, as we concluded in the last blog, regular dental visits which include x rays, are the best solution in detecting the initial signs of resorption. At that point if found, a suitable treatment can be put forward.
Yours in dental health,
Dr. F. Keshavarz Dentistry, Brampton Dentist
For any dental questions or concerns, please give us a call today @ 905.791.3867…you’ll be glad you did!
Based in Brampton, Ontario, Brampton Dentist Dr. F. Keshavarz Dentistry has been practicing gentle and pain-free dentistry for over two decades. During this time, they have helped to improve the dental health of countless satisfied patients in Peel Region, Brampton and beyond!